Medical Case: An unexplained shortness of breath, and a surprising discovery
An 82-year-old patient complains of severe shortness of breath and other symptoms, and the cause remains unclear at first. What could be behind these symptoms?
A mysterious case of breathing difficulties
An 82-year-old man presented to the emergency room with nausea, vomiting, dizziness and breathing difficulties. His medical history included the following diagnoses:
- high blood pressure
- hypothyroidism
- prediabetes
- benign prostatic hyperplasia
- dizziness and anxiety
During the further examination, the patient was asked about pain in the chest, head or abdominal area, heart palpitations, coughing and fever. He denied all of these. There was no swelling in the ankle area. He had not had any significant surgical procedures in the past. There was no alcohol or drug abuse. The patient had no known drug allergies. At the time of his presentation to the emergency room, he was taking the following medications:
- Amlodipine
- Clonazepam
- Levothyroxine
- Tamsulosin
In addition to the significant breathing difficulties already reported, the patient's physical examination revealed gasping, choking and stridor. Oxygen saturation had already dropped to 90%. The patient had become increasingly tachycardic, with a heart rate of 120 beats per minute. Auscultation of the lungs revealed coarse bubbling rales. Examination of the gastrointestinal, neurological and cardiovascular systems, however, was unremarkable. Due to the increasingly severe shortness of breath, the patient had to be intubated immediately and mechanically ventilated.1
The subsequent laryngoscopy did not clarify the symptoms. This examination method did not reveal any abnormalities. A pulmonary embolism was ruled out by means of a chest CT scan.1
Findings:
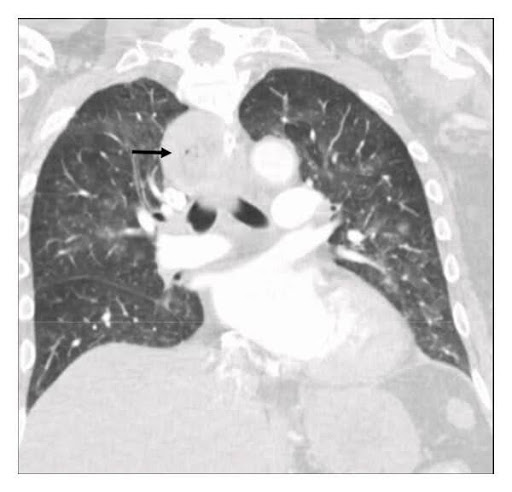
Fig. 1: CT thorax1
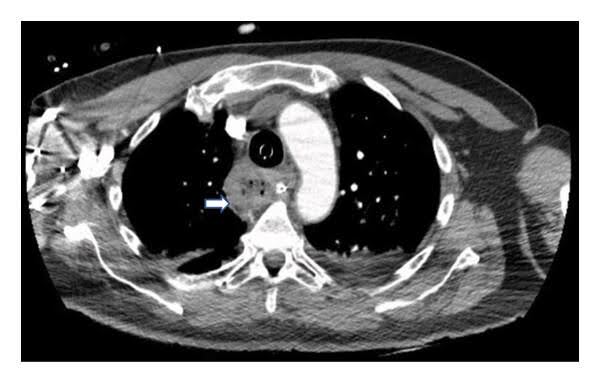
Fig. 2: CT thorax1
Here, an almost complete atelectasis of the left lower lobe and a distended oesophagus were seen. The next step was a gastroscopy to get to the bottom of the matter.
Gastroscopy results:
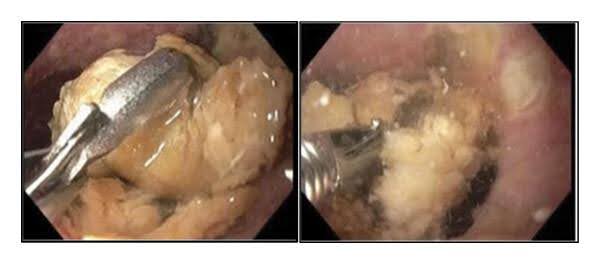
Fig. 3: Gastroscopy1
What is your suspected diagnosis, and what treatment do you suggest?
Find out if you were right:
The 82-year-old patient suffered from an oesophageal bezoar located in the lower oesophagus. It was not possible to remove the bezoar with the help of Raptor forceps and Talon grasping forceps. Bronchoscopy was performed, revealing purulent secretions and food debris in both lungs. Due to the patient's advanced age and comorbidities, surgical intervention was not initially considered. The next treatment attempt was based on direct irrigation of the oesophageal bezoar with carbonated fluids (Coca-Cola) infused with pancreatic enzymes (KREON).
At this point, the patient was endotracheally intubated, which minimised the risk of tracheal aspiration. The treatment was carried out for a total of four days (4 x daily (355 ml) Coca-Cola and 4 capsules of KREON). This led to the complete dissolution of the oesophageal bezoar. Unfortunately, oesophagitis with circumferential ulcerations remained. A hiatal hernia measuring 5 cm was also present. A biopsy ruled out eosinophilic oesophagitis.1
Findings after initiation of treatment (5th day):
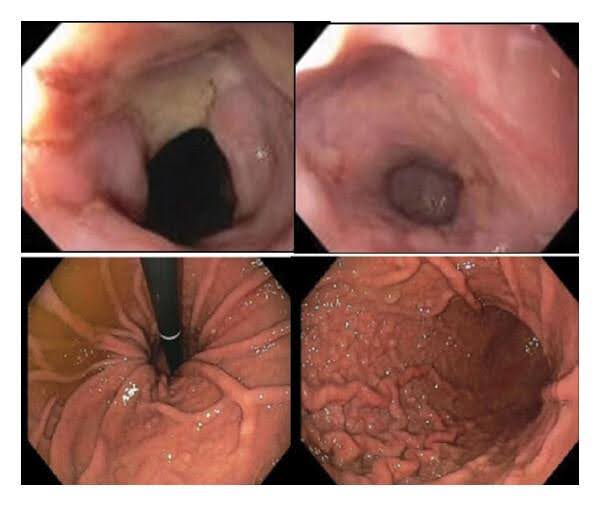
Fig. 4: Findings on the 5th day after initiation of treatment1
The patient's condition continued to improve, and he was successfully weaned from mechanical ventilation on the 6th day after initiation of treatment. At discharge, high-resolution oesophageal manometry showed type I achalasia. The patient was prescribed proton pump inhibitors in addition to his existing medication, as well as appointments for outpatient follow-up, further diagnostics and treatment of the achalasia and oesophagitis.1
Rare and potentially life-threatening: oesophageal bezoar
This rare phenomenon is characterised by the formation of a mass or foreign body in the oesophagus. In addition to the case described here, an oesophageal bezoar can also be asymptomatic. In the 82-year-old patient, the oesophageal bezoar became life-threatening due to obstruction of the upper respiratory tract.1
- Urlapu KS. et al. (2024). Severe Airway Obstruction Caused by Esophageal Bezoar with Coca-Cola and Creon (Pancrelipase) in a Patient with Underlying Achalasia: A Comprehensive Case Report. Case Rep Gastrointest Med. 2024 Jul 27;2024:2081040.



