Medical Case: A long hospital stay with recurrent infections
A 55-year-old woman suffers paraplegia, anemia, and recurrent infections. What is the underlying diagnosis?
A woman with sudden neurological symptoms
Maria T., a 55-year-old woman, was admitted to the neurosurgery unit in March due to flaccid paraplegia of the lower limbs, with tactile-pain anesthesia at the D6 level. No signs of rigidity or confusion were noted, and she did not report any additional complaints.
Physical examination
- General condition: febrile, asthenic.
- Neurological assessment: flaccid paraplegia of the lower limbs with sensory level at D6.
- Respiratory system: mildly labored breathing.
- Skin and mucosa: pallor indicative of anemia.
Medical history
Since January, Maria had experienced low-grade fever and progressively worsening back pain, which she managed at home with non-steroidal anti-inflammatory drugs and corticosteroids (up to 25 mg of prednisone daily). By February, she developed significant neurological deficits, including progressive lower limb weakness and sensory impairment, persistent severe back pain despite treatment, and ongoing fever. This is the summary of her clinical history:
- Type 2 diabetes on insulin therapy;
- history of thyroidectomy for multinodular goiter;
- previous episodes of renal colic due to nephrolithiasis;
- uninvestigated microcytic hypochromic anemia;
- prior deep vein thrombosis of the right femoropopliteal axis.
Laboratory findings
- Neutrophilic leukocytosis (WBC 14,980/μl, 74% neutrophils).
- Microcytic anemia (Hb 10.6 g/dL, MCV 75 fL).
- Elevated inflammatory markers (CRP 37.54 mg/dL, ESR 72 mm/h).
- Normal thyroid function tests with replacement therapy.
- Hyperglycemia (225 mg/dL).
Clinical and diagnostic approach
Spinal MRI with contrast revealed destruction of the D3-D4 intervertebral disc, osteolytic lesions of the vertebral bodies, and high signal intensity on STIR sequences, indicative of an inflammatory process with associated epidural and pleural abscess formation.
A CT-guided biopsy was performed both for therapeutic drainage of the purulent collection and for diagnostic purposes, with sampling of paravertebral and pleural material. Cultures of the exudate tested positive for Staphylococcus aureus. Empirical antibiotic therapy was initiated with teicoplanin 600 mg/day, followed by rifampicin 600 mg/day and levofloxacin 500 mg/day.
FDG-PET was performed to assess disease extent and aid in therapeutic monitoring. The scan confirmed an inflammatory focus at D3-D4, along with nonspecific areas of uptake in the sigmoid colon and rectum. Neurosurgeons deemed surgical stabilization unnecessary due to the chronicity of the neurological deficits and the patient’s overall poor condition, which included prolonged immobility, obesity, and dependence on total parenteral nutrition due to poor oral intake. Chronic opioid therapy was being used to manage thoraco-abdominal neuropathic pain.
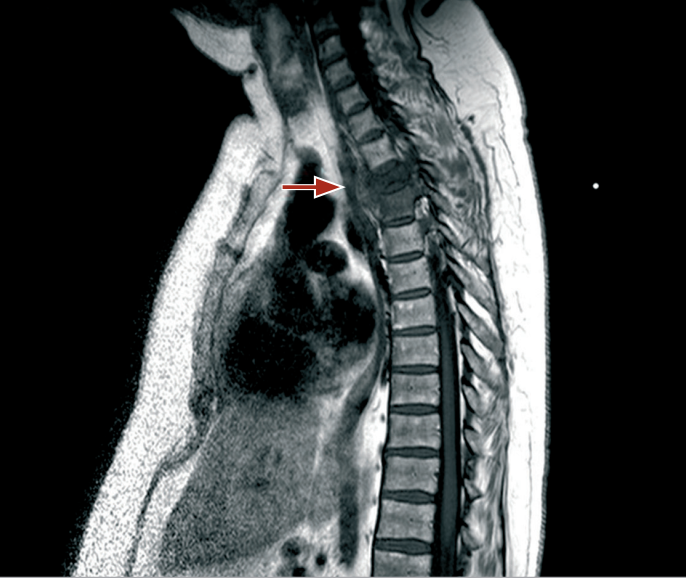
MRI of the spine with contrast agent: hypodensity of the vertebral body can be seen at T1
Transfer to Internal Medicine
In April, Maria was transferred to the Internal Medicine department due to persistent hyperpyrexia. Chest X-ray, abdominal ultrasound, and urinalysis showed no clear infectious foci. Given her complex medical background, transthoracic echocardiography was performed, ruling out valvular vegetations. Blood cultures taken after the removal of a central venous catheter (CVC), which appeared slightly erythematous at the insertion site, tested positive for Staphylococcus epidermidis and Escherichia coli.
In July, during her prolonged hospitalization, she developed acute respiratory failure secondary to Candida albicans pneumonia.
By September, she again exhibited low-grade fever and worsening microcytic sideropenic anemia with depleted iron stores: Hb = 7.7 g/dL, MCV = 70 fL, CRP = 15 mg/dL, WBC = 13,800/μL, serum iron = 13 μg/dL, and ferritin = 200 ng/mL. Occult blood was detected in three stool samples.
What is your suspected diagnosis, and what treatment do you suggest?
Find out if you were right:
Diagnosis of hidden pathology
A PET scan is performed (scheduled as a check-up six months after the first diagnosis). The tracer is no longer fixed dorsally, but only at the level of the walls of the large intestine, which appeared elongated beyond normal.
Based on these haemato-instrumental data, endoscopic examinations (gastroscopy and colonoscopy) are performed and the determination of calprotectin (tested positive with a value of 72 g/kg). The typical lesions found at the colonoscopy first and at the histology of the colic mucosa biopsy later, allowed Crohn's disease to be diagnosed.
Coping with misleading diagnoses
This clinical case is intended to illustrate how the definitive diagnosis is often obtained after a long period punctuated by complications, which can be misleading. In this patient, the cause of the origin of the numerous infections, microcytic and sideropenic anaemia, spondylodiscitis and numerous pneumonias is ultimately attributed to a chronic inflammatory disease, Crohn's disease: the ulcerated colic lesions are the site of the origin of the septic foci.
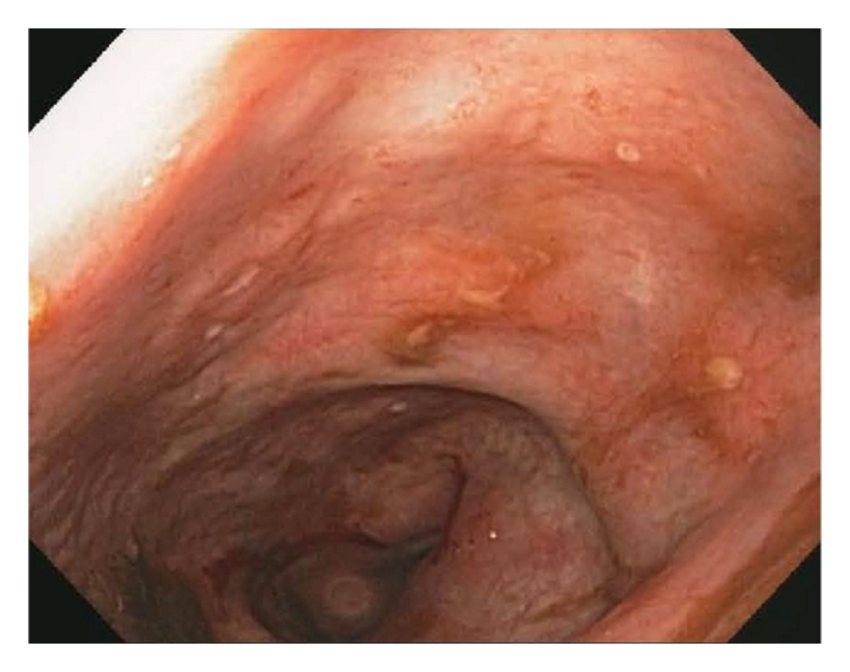
Endoscopic features of Crohn’s disease. Photo credits5
Insights and useful resources
- Zoppis E. A hidden pathology: Crohn disease. CMI 2011; 5(Suppl 2): 59-64
- Sobottke R, Seifert H, Fätkenheuer G, Schmidt M, Goßmann A, Eysel P. Current diagnosis and treatment of spondylodiscitis. Dtsch Arztebl Int 2008; 105: 181-7
- Gratz S, Dörner J, Fischer U, Behr TM, Béhé M, Altenvoerde G et al. 18F-FDG hybrid PET in patients with suspected spondylitis. Eur J Nucl Med 2002; 29: 516-24
- Ozuna RM, Delamarter RB. Pyogenic vertebral osteomyelitis and postsurgical disc space infections. Orthop Clin North Am 1996; 27: 87-94
- Hamilton MJ. The valuable role of endoscopy in inflammatory bowel disease. Diagn Ther Endosc. 2012;2012:467979. doi: 10.1155/2012/467979. Epub 2012 Feb 29. PMID: 22474403; PMCID: PMC3299364.

